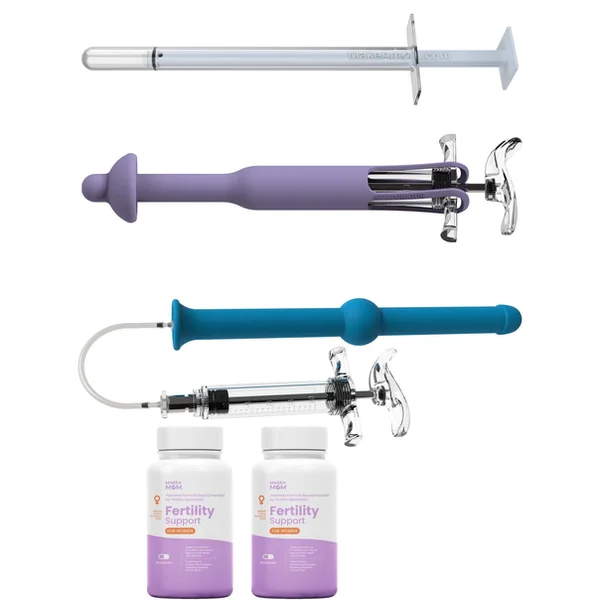
Her Success Kit (19-Piece Complete Bundle)
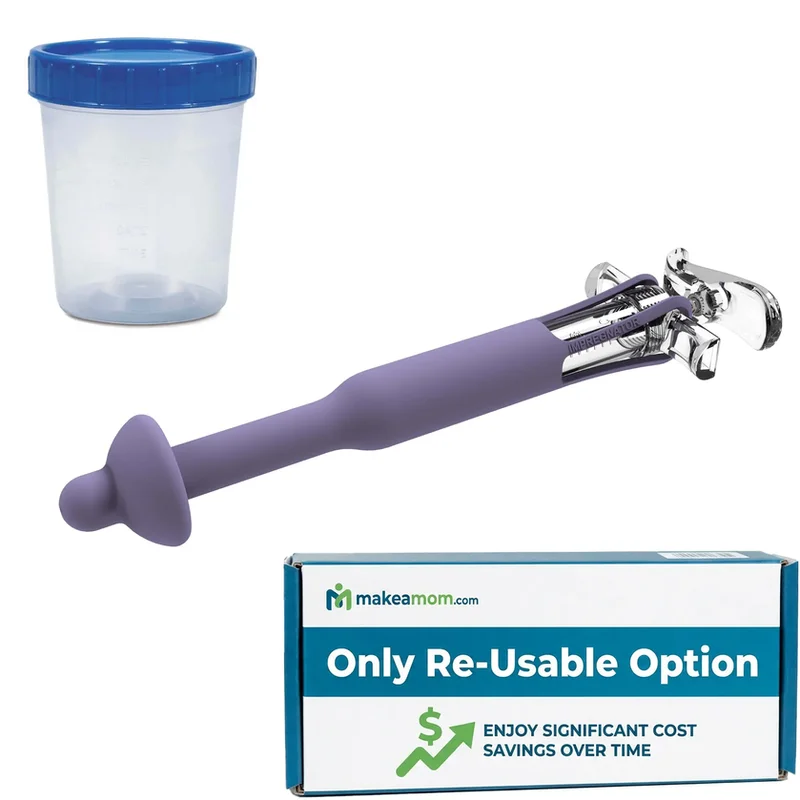
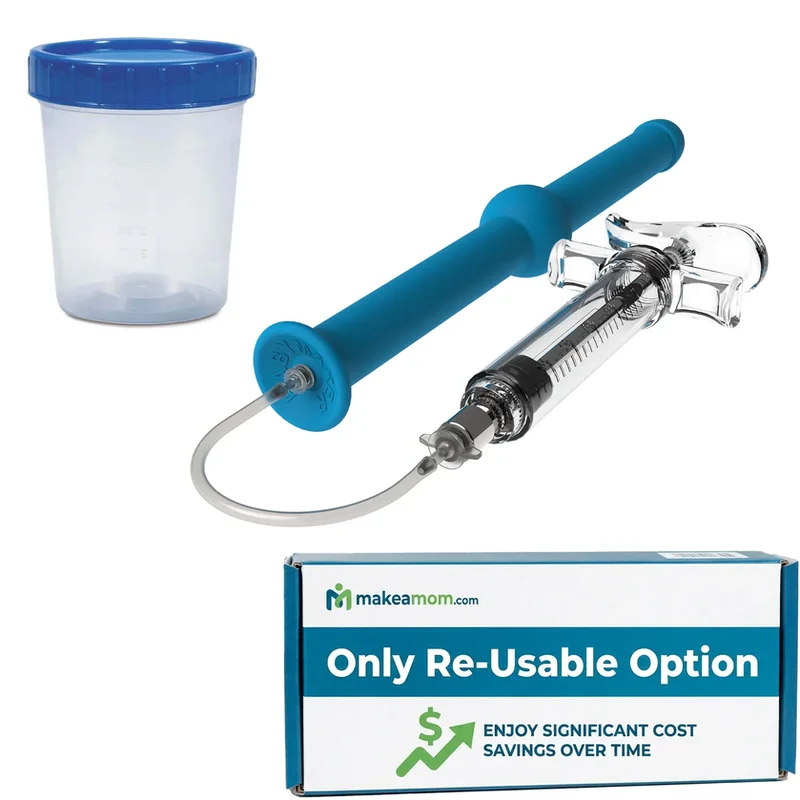
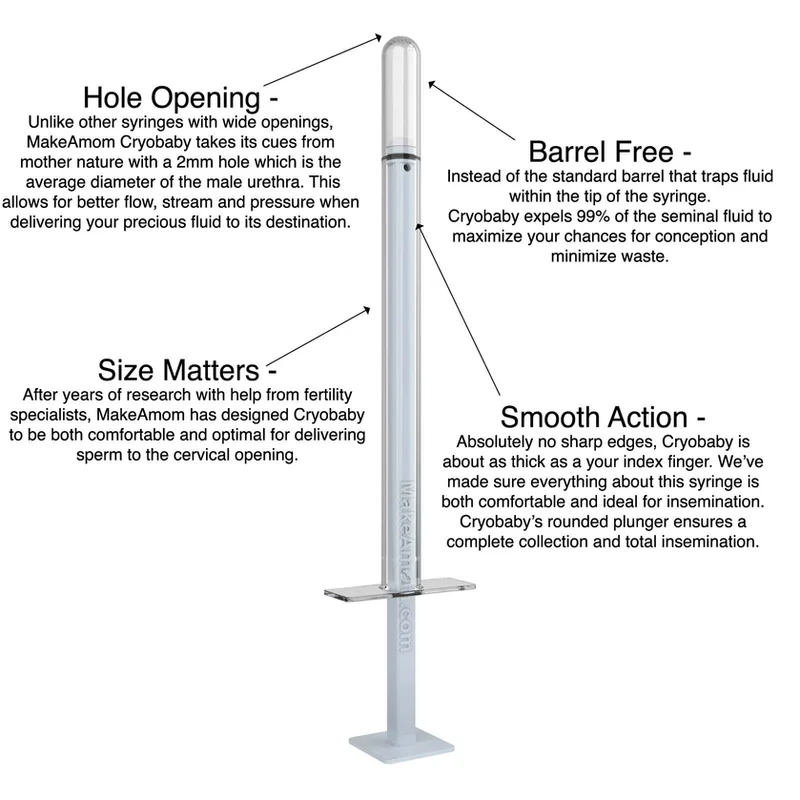
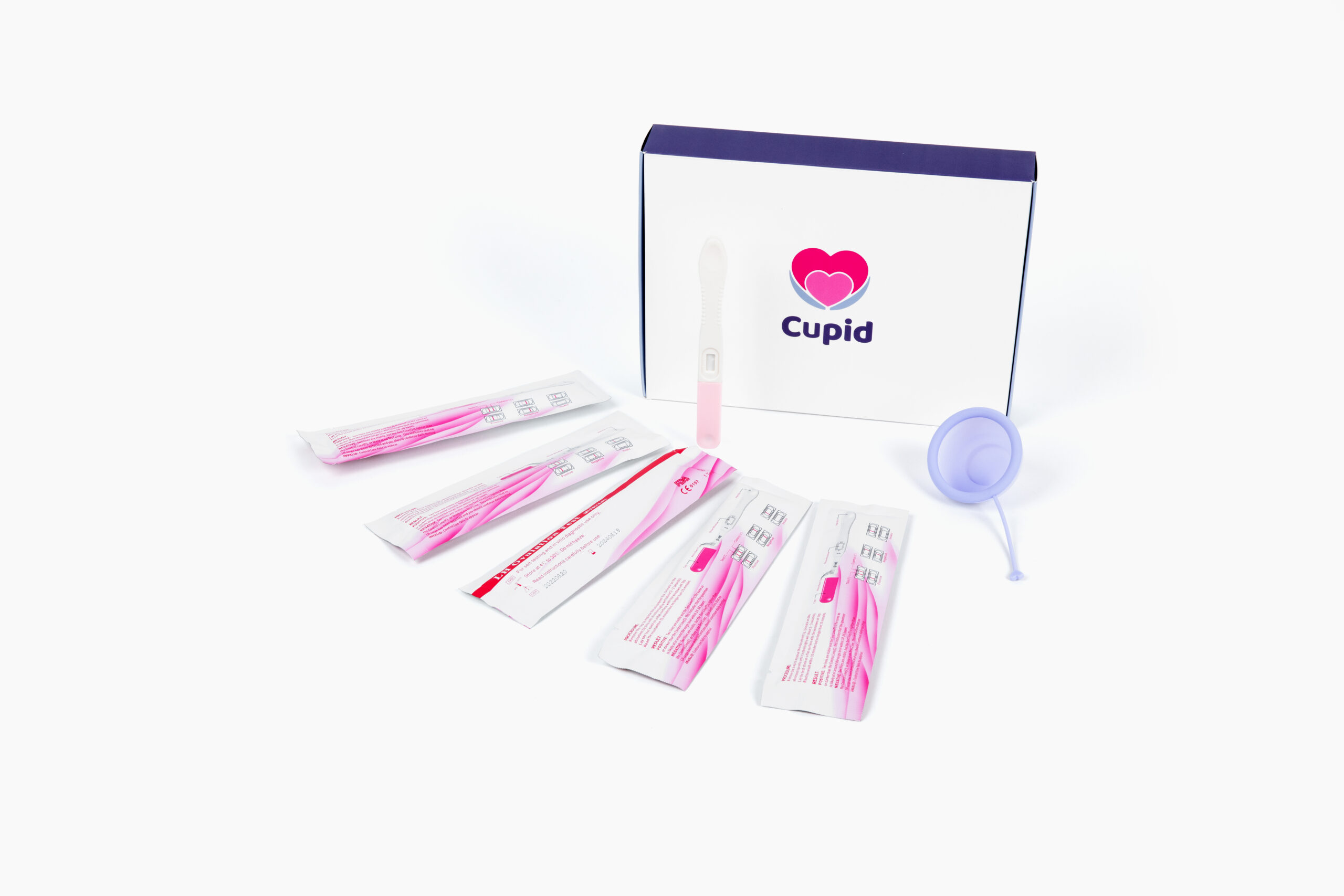
The most comprehensive at-home insemination kit available. Includes all three MakeAMom devices (Impregnator, BabyMaker, CryoBaby), fertility supplements, ovulation and pregnancy test strips, and a detailed guide. Designed for maximum versatility across fresh and frozen samples.